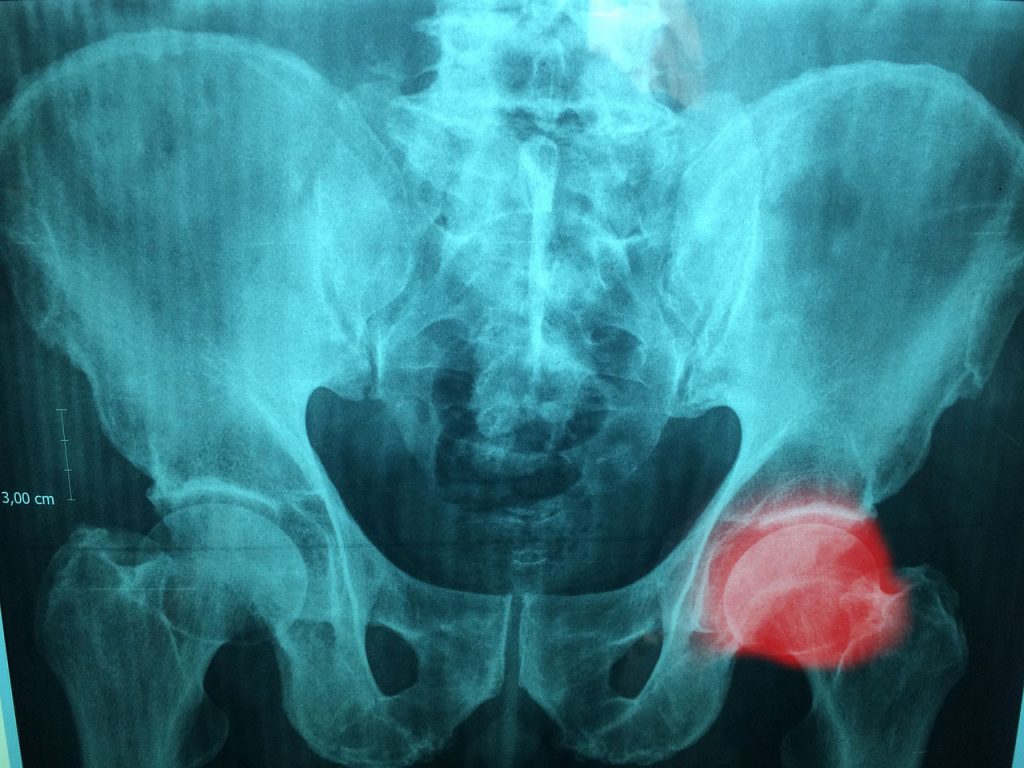
Now that I finished, those two are back with a vengeance, along with the neuropathy,” shared a MyOvarianCancerTeam member. “Having rheumatoid arthritis and fibromyalgia, those symptoms seemed to take a back seat to chemo. Knowing your family history can help identify risk factors for these other health conditions. People with ovarian cancer can experience hip pain for lots of reasons, many unrelated to their cancer, including:
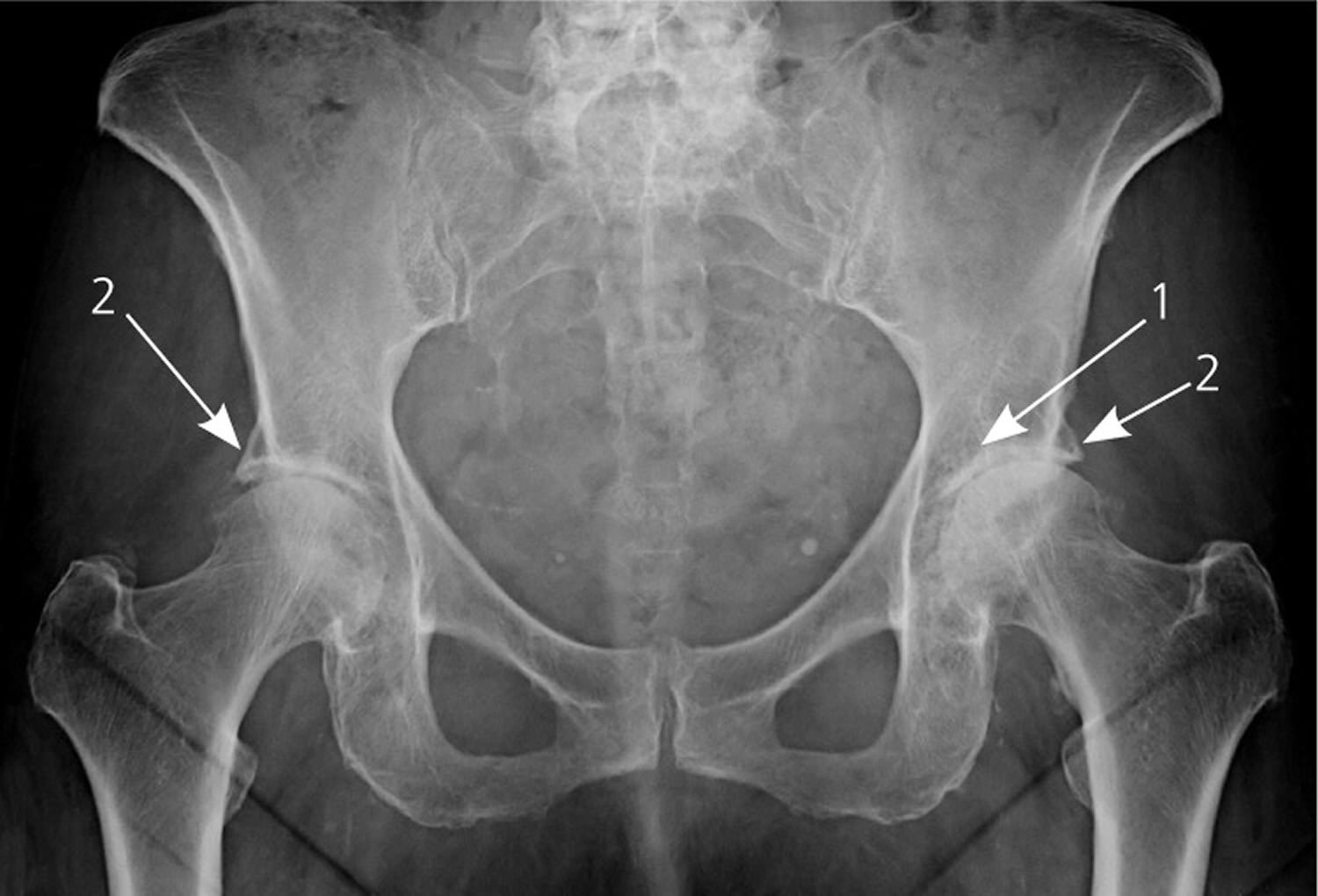
Ask your doctor if any side effects of your treatment may be responsible for your hip pain. Ironically, bisphosphonates - which are used to treat bone loss - and some pain medicines also can cause joint pain. Targeted cancer therapies including olaparib ( Lynparza).Aromatase inhibitors and other hormonal therapies used in breast cancer.□”Īccording to the American Society of Clinical Oncology, some people also experience joint pain as an immediate or late side effect of cancer treatments. I decided to get back into tai chi, and it’s helped! I don’t have the stamina yet to do the complete hour, but I’m working on that. I was told that arthritis can become worse with chemo. One MyOvarianCancerTeam member wrote, “Has anyone experienced post-chemo pain? It’s mainly in my bones and joints. When deciding on treatments, your oncologist will weigh the benefits and risks to give you the best possible cancer care. It’s not always possible to predict or prevent these issues, but doing your best to stay active, eat well, and follow other healthy lifestyle habits before and after cancer can help. Chemotherapy can also cause nerve damage, and immunotherapy can affect muscles and joints. “I have osteoporosis from my cancer drugs, so I’ll have to have an IV once a year for 30 minutes to help with my bones,” one member explained.Ĭhemotherapy, radiation, and hormone therapy are all potential contributors to osteoporosis later in life. For example, several members of MyOvarianCancerTeam report experiencing osteoporosis (weak, brittle bones) and bone fractures. Treatment for ovarian cancer may lead to side effects that increase your risk of hip pain. Fortunately, ongoing monitoring by your health care team can prompt the early detection of any new problems. If you remember having pain with your undiagnosed ovarian cancer, it’s understandable to worry when other sources of pain arise. “I haven’t had a minute of back pain since my hysterectomy.” I had cancer in both ovaries, tubes, and my uterus,” shared one member. I thought it was scar tissue from three cesarean sections. Then I started having menstrual cramps at 67 years old. I tried physical therapy and a chiropractor. However, pain isn’t always a clear indicator of the disease. Members of MyOvarianCancerTeam have described how pain and cramping were early signs of ovarian cancer. But overall, researchers consider it extremely rare for ovarian cancer to spread to bone. If ovarian cancer spreads to the bone (such as the pelvis or hip bones), pain is one of the most reported symptoms. The most likely areas for ovarian cancer to spread include the liver, spleen, intestines, brain, skin, lymph nodes, and the fluid around the lungs. However, it’s important not to jump to conclusions about hip pain. If you’re living with ovarian cancer and you feel an unexpected pain sensation, it’s normal to worry that cancer may be growing or spreading. Here are some possible causes of hip pain that may or may not be associated with ovarian cancer, along with tips for when to seek treatment and how to manage discomfort.
